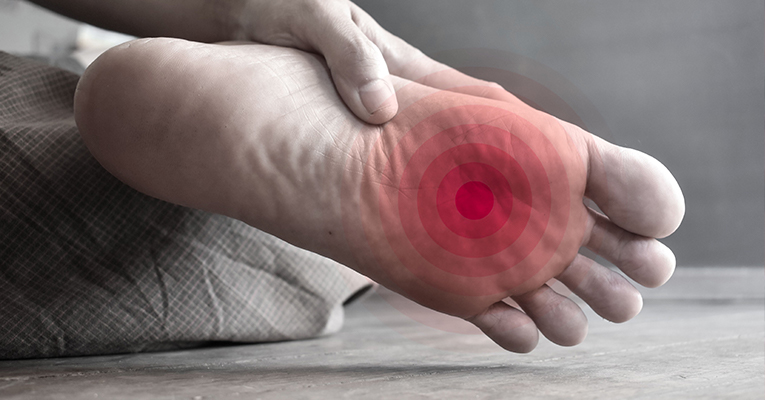
Bacteria invade your skin when it is damaged or cracked. Scrapes, burns, surgeries, fungal infections, and other factors can all cause skin breaks. Bacteria can enter even if the breach in the skin is just too small to see. Cellulitis can impact any area of the body, although it is most commonly found in the limbs. It typically manifests as red patches, soreness, swelling, and burning, and it can also result in a fever. Cellulitis and diabetics are more relatable when it comes to diabetes; and are more common in the summer, probably because the heat produces greater perspiration and swelling, resulting in skin irregularities. If you feel you have cellulitis, see your doctor as soon as possible.
If microorganisms enter the layers of skin, anybody can have a potentially severe skin infection. Certain factors, however, increase your chances of acquiring cellulitis even more worse in the case of diabetes.
Cellulitis symptoms include swelling, redness, soreness, and tenderness in the afflicted region. Blisters, shivers, fevers, and nausea are also common. Antibiotics can be used to treat cellulitis. However, if left untreated, the bacteria can affect the blood system and prove fatal. Although cellulitis is not always prevented, recognizing its causes and consequences may reduce your chances of contracting this infection.
The immune response is the mechanism through which the body manages infection. When the immune system is weakened, the ability to regulate infection is reduced, allowing bacteria to multiply and cause damage. People with weakened immune systems, such as those affected by cancer, HIV/AIDS, or even certain drugs, should take extra care to keep their skin clean in order to avoid cellulitis; especially cellulitis in diabetes. For example, one basic step to take is to keep the crevices between the toes dry and clear of infection. Cleansing scratches with soap and warm water, applying moisturizer to dry skin, and cleaning your hands frequently are some methods to practice excellent skin hygiene.
Whether you have diabetes, you are more likely to develop cellulitis in diabetes in two ways. The first is connected to diabetic problems. Diabetic neuropathy (nerve damage) is a frequent diabetic consequence that causes you to lose feeling, particularly in your feet. This implies that if you have a leg injury or diabetic leg cellulitis, you may well not recognize it – which makes it difficult to treat effectively, allowing bacteria to enter.
The second way diabetes raises the risk of cellulitis is that elevated blood sugar, which is a characteristic of diabetes, impairs immune function, allowing bacterium and other infectious microbes to proliferate.
If you have diabetes, you may help prevent yourself from cellulitis by always wearing comfortable shoes and protective gloves when appropriate. You should also keep an eye out for any indications of illness. Therefore, patients with diabetes (chances of cellulitis), especially, should seek medical attention if they do not notice symptoms of wound repair in a day or two.
Pre-existing skin problems like athlete’s foot allow skin germs to reach greater depths of the skin and produce infection. The athlete’s foot is distinguished by blistering, cracking, or peeling skin beneath your foot, which allows germs to enter the skin and the tissues beneath it. Cellulitis other than in diabetes, is also more likely if you have eczema. The skin condition indicates that your skin’s barrier has been damaged, but you may have more germs on your skin than usual, both of which might lead to infection.
Lymphedema is a chronic disorder that causes swelling. It impairs the lymphatic system, which is critical in assisting your body in fighting sickness. Lymphatic fluid, which transports anti-infection white blood cells, accumulates in the legs and arms. This condition increases your chances of acquiring cellulitis and so in diabetes when there is cellulitis. The accumulation of fluid in afflicted areas causes edema and can create skin abnormalities that predispose to infection. Once germs infiltrate the skin and soft tissue, the lymphatic fluid provides an ideal environment for them to proliferate. Furthermore, the lymphatic system’s dysfunction makes it less capable of fighting infection.
Anything that generates a breach in the skin, such as a cut or abrasion, provides a chance for skin germs to infiltrate deeper. Take care to wash and disinfect any wounds or scrapes and to keep a lookout for any indications of infection. Bed sores might also make you susceptible to infection.
The veins within your legs normally maintain blood flowing toward your heart. However, with venous insufficiency, all connections in these veins are broken, allowing blood to flow backward into the legs. This leads blood to pool and build up in the legs, causing discomfort, swelling, and, in severe instances, open sores. Because these lesions are open places through which bacteria may readily infiltrate the deep layers of the skin, they render persons with venous insufficiency particularly susceptible to cellulitis and so in the case of diabetes.
See Also: Diabetes Cellulitis Treatment – How to Diagnose and Treat It?