In an autoimmune disease, the body’s immune system attacks the body itself. An autoimmune disease can affect many areas of the body, including the joints, bones, or tissues. One common organ that autoimmune diseases attack is the skin and such a disease is known as an autoimmune skin disease. In a study conducted in 2019, 262 out of the 1,000,000 patients who came to public skin clinics in Botswana were diagnosed with an autoimmune skin disease.
The skin is the largest organ of the body and makes up sixteen percent of total body mass. It plays a significant role in protecting the body against different types of infections which is why it is considered a part of the immune system. For example, the skin has Langerhans cells that play a vital role in fighting the body against disease-causing microbes or pathogens. It also offers a protective layer against injuries that could be physical, mechanical, thermal, or against harmful substances. It helps regulate body temperature and stabilizes other body processes, such as homeostasis.
The skin mainly comprises three layers, the outermost is called the epidermis, beneath that is the dermis, and the innermost one is called the hypodermis. Many proteins lie in between these layers and hold them together. Autoimmune skin diseases usually affect the top two layers of the skin.
Some examples of common autoimmune skin conditions include:
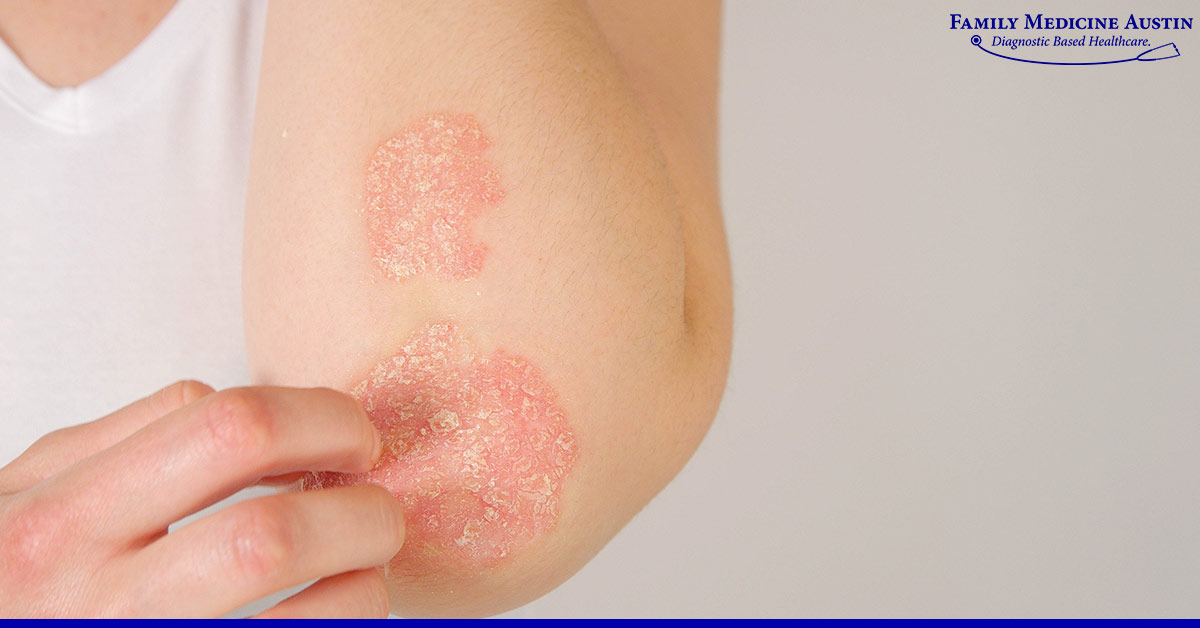
Characterized by an overactive immune system, psoriasis is an autoimmune skin disorder that is also chronic. The growth of skin cells becomes sped up, which is why they begin to form deposits on the skin and results in scales that are red plaques covered with white patches of dead skin. These plaques can appear anywhere on the body from the scalp, elbow, lower back, elbows, or knees. In 2013 alone, 7.4 million Americans become a victim of skin disorders.
Scleroderma does not only show its symptoms on the skin (localized scleroderma) but also affects other parts of the body, such as the blood vessels, muscles, and organs, such as the heart, lungs, and kidneys (systemic scleroderma). 300,000 Americans have the disease, and out of these, one-third have scleroderma of the systemic type. 80% of patients suffering from the disease are females.
Dermatomyositis affects the muscles and the skin. One of its most prominent symptoms is a skin rash that appears on the top part of the body. It also causes eyelids to become purple and skin to become thick.
Lupus is another chronic autoimmune skin disease. There are different types of skin lupus. Cutaneous lupus mainly affects the skin, while other parts of the body, such as the kidneys, joints, and heart can be affected too. In systemic lupus, the blood vessels get affected. It usually affects women between the age of 15 to 44.

In the United States, Behcet’s Disease occurs in 7 out of 100,000 persons. Characterized by the inflammation of blood vessels all over the body, Bechet’s Disease is a rare disorder. Its symptoms include inflammation of the eyes, rashes, and genital lesions. The severity of the symptoms varies from person to person, and while the disease has no cure to it, treatment can help manage the symptoms. Patients may also go through remission when symptoms reappear.
Pemphigus is a group of autoimmune skin diseases that show their symptoms in the form of blisters. Usually, blisters start to appear in the mouth and then spread to the rest of the body. While some people have blisters on some parts of the skin, others may get them on larger parts. These blisters may form ulcers that join on the skin and cause a lot of pain. Pemphigus rarely occurs in children and is more common in people aged 40 to 60.
Some other common autoimmune skin conditions include:
While autoimmune diseases do not show their signs or symptoms immediately, autoimmune skin diseases are easy to detect as they become apparent on the skin.
General symptoms of autoimmune skin diseases include:
If you are concerned about whether an autoimmune skin disease will cause permanent changes to the skin, don’t worry, since most symptoms on the skin are temporary. Only in the case of discoid lupus erythematosus, does permanent scarring, discoloration, or hair loss may occur. In some kinds of bullous pemphigoid, permanent scars may appear on the skin or the mouth, eyes, and throat.
Scientists and researchers believe that certain triggers cause the body’s immune system to attack itself. These triggers include:
Furthermore, researchers believe some people have genes that increase the chances of an autoimmune disease, but only if the trigger factors exist in the first place.
Since an autoimmune skin disease occurs because of the immune system attacking itself, the best way to treat the disorder is to suppress the immune system. Doctors prescribe medicine to block inflammation and suppress the immune system. Some of these medicines include:
Doctors usually prescribe medication in the form of lotions or creams if small areas of the skin get impacted by the autoimmune skin disease. Otherwise, they prescribe pills or injections.
Autoimmune Skin Diseases and Protection from the Sun
Sun damage is generally bad for the skin since it causes wrinkling, spots, and aging. People suffering from an autoimmune skin disease should be even more careful about protecting themselves from the sun as their skin cells are already damaged. Such people should wear sunscreen of at least SPF 30 at all times, and minimize exposure to the sun.
Psoriasis may require phototherapy, in which a technician exposes them to ultraviolet radiation for treatment. Some autoimmune skin diseases medication may also make patients more vulnerable to the radiation of the sun.
Treating an autoimmune skin disease is essential since leaving rashes, blisters, or open sores untreated may lead to severe itching and pain. You may experience discomfort and scarring may occur. Henceforth, it is best to go to a doctor at the earliest. Family Medicine Austin offers testing services for autoimmune skin diseases. Get yourself tested so our technicians can prescribe you the appropriate medication for it.